
At Pain Psychotherapy Canada, we specialize in treating chronic pain & symptoms.
Education on Neuroplastic Pain & Symptoms
Studies have shown that chronic pain and symptoms such as back pain, fibromyalgia, pelvic pain, neck pain, migraines, headaches, IBS, fatigue, dizziness, and tinnitus are often not physically caused, but occur in the brain due to learned neural pathways 1,2. This condition is called neuroplastic pain or symptoms.
At Pain Psychotherapy Canada, we specialize in treatment approaches that reduce or eliminate neuroplastic pain and symptoms. We know this is possible because our therapists have helped hundreds of clients achieve it, and research has found it is possible 2,3.

The following factors can trigger and perpetuate neuroplastic pain and symptoms 8:
-
Belief the body is permanently damaged or flawed
Responding to our pain or symptoms with fear, worry, frustration, despair, grief, or anger
Anxious and depressive symptoms
Unprocessed trauma impacting nervous system functioning
Nervous system dysregulation, meaning being stuck in a fight, flight, freeze, or shutdown state for prolonged periods of time
High-alert behaviours such as perfectionism, people-pleasing, placing pressure on ourselves, excessive control, self-criticism, worrying, and/or obsessive thinking
Social and environmental factors that create a sense of danger
Our Treatment Approach
To help our clients reduce or eliminate pain, our treatment approach utilizes tools and education from Pain Reprocessing Therapy, Emotional Awareness and Expression Therapy, Somatic Experiencing, Polyvagal Theory, and other cognitive, somatic, behavioural, and trauma-focused therapies.
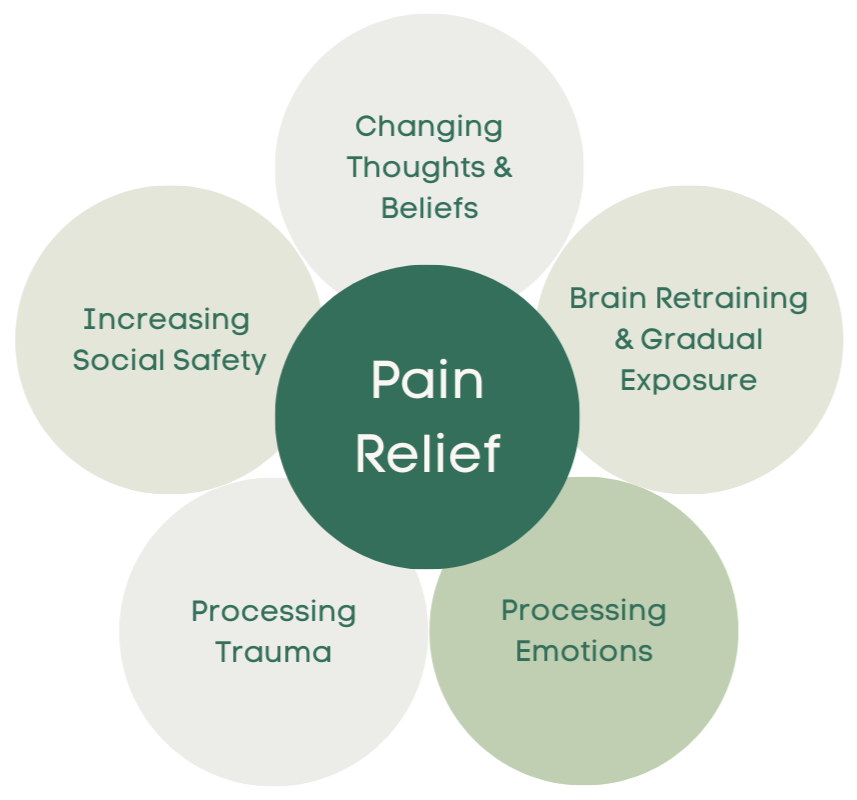
We use a detailed and holistic approach focused on 5 main areas:
-
Gathering evidence for physical safety:
Our work begins with an assessment for the likeliness of neuroplastic pain and symptoms. We engage in a detailed assessment, where we look for signs that a client’s pain or symptom is not behaving in ways consistent with a structural injury or disease.
Looking for signs your pain or symptom is neuroplastic is a very important step toward creating safer beliefs about your body, as you understand your body is safer and more capable than you once thought 6.
Developing safer thinking patterns and beliefs
Chronic pain and symptoms invite the mind to think negatively. Many of our clients experience fixation on their symptoms, negative views about their bodies, worry about the future, fear of activities that may cause pain, self-judgment, and spend a lot of time trying to diagnose or find a cure.
We help our clients shift toward more helpful, hopeful, compassionate, and empowered thinking habits that increase their safety and reduce symptoms.
-
Practicing safer responses to physical sensations
Strategies from Pain Reprocessing Therapy help “retrain the brain to respond to sensations from the body properly, and subsequently break the cycle of chronic pain” 6.
Somatic tracking is one of the primary techniques utilized in Pain Reprocessing Therapy, which helps clients feel safe with sensations occurring in their body. This heals the communication between mind and body, reducing pain/symptoms over time.
Reducing fear-based avoidance
The principles of exposure therapy are important in our approach. As our clients gain confidence in their body’s safety, we help them reduce avoidance and gently increase their movement, activity level, and ability to live life.
Through graded exposure, our brains gain new evidence for safety by witnessing us engaging in tasks that used to feel dangerous or impossible 6. When the brain realizes it no longer needs to protect us, fear and pain/symptom sensations go extinct 6. This allows our clients to engage more fully in life again.
-
Learning to feel safe with emotions and dysregulation
Studies have found that similar areas of the brain are activated during both emotional pain and physical pain, and resisting or suppressing difficult emotions can increase pain sensations 10, 11.
When our nervous system becomes chronically dysregulated and stuck in a fight, flight, fawn, freeze, or shutdown state, we become prone to developing chronic pain, chronic fatigue, and IBS 13, 14, 15, 16.
We help our clients learn to fully feel and allow difficult emotions and dysregulation in their body, and create a sense of safety. By increasing our safety with our emotions, pain and symptoms reduce 12.
Our goal is to help our clients become fully embodied beings, where the emotions and sensations they feel in their bodies become helpful signals that can guide them toward self-expression and their values.
-
How to overcome trauma
To facilitate nervous system regulation, we help our clients process trauma, utilizing Somatic Experiencing, Somatic Attachment, Accelerated Resolution Therapy (ART), EMDR, Radical Exposure Tapping, and Prolonged Exposure Therapy.
These approaches help our clients process memories and reduce the cognitive and emotional impacts of past events, leading to reduced nervous system reactivity and greater safety. A safer and more regulated nervous system experiences less chronic pain and symptoms.
-
Improving Relationships
Experiencing concerns with attachment, conflict, loneliness, boundaries and abuse can create a sense of danger in our mind and body, causing and amplifying pain/symptoms 27.
We utilize systemic approaches to help our clients increase safety and improve relationships with family, intimate partners, friends, and workplaces.
Addressing the impacts of systemic oppression
Chronic stress from oppression of our body, sexuality, gender, racial identity, cultural differences, and/or neurodiversity can cause and amplify pain 28,29.
We utilize affirming and anti-oppressive counselling approaches to help our clients develop a sense of safety within their bodies and identities, navigate oppression, and increase their social safety to improve mental health and reduce pain.
To begin your journey out of chronic pain and symptoms, schedule a free 20-minute consultation with one of our therapists!
Woolf C. J. (2011). Central sensitization: implications for the diagnosis and treatment of pain. Pain, 152(3 Suppl), S2–S15. https://doi.org/10.1016/j.pain.2010.09.030
Ashar, Y. K., Gordon, A., Schubiner, H., Uipi, C., Knight, K., Anderson, Z., Carlisle, J., Polisky, L., Geuter, S., Flood, T. F., Kragel, P. A., Dimidjian, S., Lumley, M. A., & Wager, T. D. (2022). Effect of Pain Reprocessing Therapy vs Placebo and Usual Care for Patients With Chronic Back Pain: A Randomized Clinical Trial. JAMA psychiatry, 79(1), 13–23. https://doi.org/10.1001/jamapsychiatry.2021.2669
Andersen, T.E., Ellegaard, H., Schiøttz-Christensen, B. et al. Somatic experiencing® for patients with low back pain and comorbid posttraumatic stress disorder – protocol of a randomized controlled trial. BMC Complement Altern Med 18, 308 (2018). https://doi.org/10.1186/s12906-018-2370-y
Derbyshire, S. W., Whalley, M. G., Stenger, V. A., Oakley, D. A. (2004) Cerebral activation during hypnotically induced and imagined pain. Neuroimage, 23(1), 392-401.
Gordon, A., Ziv, A. (2021). The way out: A revolutionary, scientifically proven approach to healing chronic pain. Sony/ATV Music Publishing LLC.
Pain Reprocessing Therapy Center (2021). Pain reprocessing therapy training.
Crofford LJ. Chronic Pain: Where the Body Meets the Brain. Trans Am Clin Climatol Assoc. 2015;126:167-83. PMID: 26330672; PMCID: PMC4530716.
Dana, D. (2018). The polyvagal theory in therapy: Engaging the rhythm of regulation. WW Norton & Co.
Hashmi, J. A., Baliki, M. N., Huang, L., Baria, A. T., Torbey, S., Hermann, K. M., Schnitzer, T. J., & Apkarian, A. V. (2013). Shape shifting pain: chronification of back pain shifts brain representation from nociceptive to emotional circuits. Brain : a journal of neurology, 136(Pt 9), 2751–2768. https://doi.org/10.1093/brain/awt211
Burns, J. W., Quartana, P. J., & Bruehl, S. (2008). Anger inhibition and pain: Conceptualizations, evidence and new directions. Journal of Behavioral Medicine, 31, 259 –279. http://dx.doi.org/10.1007/s10865-008- 9154-7
Kross, E., Berman, M. G., Mischel, W., Smith, E. E., Wager, T. D. (2011). Social rejection shares somatosensory representations with physical pain. Proceedings of the National Academy of Sciences of the USA, 108, 6270-6275.
Lumley, M. A., Schubiner, H., Lockhart, N. A., Kidwell, K. M., Harte, S. E., Clauw, D. J., & Williams, D. A. (2017). Emotional awareness and expression therapy, cognitive behavioral therapy, and education for fibromyalgia: a cluster-randomized controlled trial. Pain, 158(12), 2354–2363. https://doi.org/10.1097/j.pain.0000000000001036
Bonaz, B., Sinniger, V., & Pellissier, S. (2016). Vagal tone: effects on sensitivity, motility, and inflammation. Neurogastroenterology and motility : the official journal of the European Gastrointestinal Motility Society, 28(4), 455–462. https://doi.org/10.1111/nmo.12817
Pellissier, S., Dantzer, C., Mondillon, L., Trocme, C., Gauchez, A. S., Ducros, V., Mathieu, N., Toussaint, B., Fournier, A., Canini, F., & Bonaz, B. (2014). Relationship between vagal tone, cortisol, TNF-alpha, epinephrine and negative affects in Crohn's disease and irritable bowel syndrome. PloS one, 9(9), e105328. https://doi.org/10.1371/journal.pone.0105328
Koenig, J., Loerbroks, A., Jarczok, M. N., Fischer, J. E., & Thayer, J. F. (2016). Chronic Pain and Heart Rate Variability in a Cross-Sectional Occupational Sample: Evidence for Impaired Vagal Control. The Clinical journal of pain, 32(3), 218–225. https://doi.org/10.1097/AJP.0000000000000242
Van Cauwenbergh, D., Nijs, J., Kos, D., Van Weijnen, L., Struyf, F., & Meeus, M. (2014). Malfunctioning of the autonomic nervous system in patients with chronic fatigue syndrome: a systematic literature review. European journal of clinical investigation, 44(5), 516–526. https://doi.org/10.1111/eci.12256
Schneider, M., & Schwerdtfeger, A. (2020). Autonomic dysfunction in posttraumatic stress disorder indexed by heart rate variability: a meta-analysis. Psychological medicine, 50(12), 1937–1948. https://doi.org/10.1017/S003329172000207X
Dana, D. (2019). 2-Day Workshop: Polyvagal Theory Informed Trauma Assessment and Interventions
Elbers, J., Jaradeh, S., Yeh, A. M., & Golianu, B. (2018). Wired for Threat: Clinical Features of Nervous System Dysregulation in 80 Children. Pediatric neurology, 89, 39–48. https://doi.org/10.1016/j.pediatrneurol.2018.07.007
Kanthak, M. K., Stalder, T., Hill, L. K., Thayer, J. F., Penz, M., & Kirschbaum, C. (2017). Autonomic dysregulation in burnout and depression: evidence for the central role of exhaustion. Scandinavian journal of work, environment & health, 43(5), 475–484. https://doi.org/10.5271/sjweh.3647
Grippo, A. J., Lamb, D. G., Carter, C. S., & Porges, S. W. (2007). Social isolation disrupts autonomic regulation of the heart and influences negative affective behaviors. Biological psychiatry, 62(10), 1162–1170. https://doi.org/10.1016/j.biopsych.2007.04.011
Afshar, H., Roohafza, H., Sadeghi, M., Saadaty, A., Salehi, M., Motamedi, M., Matinpour, M., Isfahani, H. N., & Asadollahi, G. (2011). Positive and negative perfectionism and their relationship with anxiety and depression in Iranian school students. Journal of research in medical sciences : the official journal of Isfahan University of Medical Sciences, 16(1), 79–86.
Patel, Jainish & Patel, Prittesh. (2019). Consequences of Repression of Emotion: Physical Health, Mental Health and General Well Being. International Journal of Psychotherapy Practice and Research. 1. 16-21. 10.14302/issn.2574-612X.ijpr-18-2564.
Hirotsu, C., Tufik, S., & Andersen, M. L. (2015). Interactions between sleep, stress, and metabolism: From physiological to pathological conditions. Sleep science (Sao Paulo, Brazil), 8(3), 143–152. https://doi.org/10.1016/j.slsci.2015.09.002
Mulkey, S. B., & du Plessis, A. J. (2019). Autonomic nervous system development and its impact on neuropsychiatric outcome. Pediatric research, 85(2), 120–126. https://doi.org/10.1038/s41390-018-0155-0
Pyhälä, R., Wolford, E., Kautiainen, H., Andersson, S., Bartmann, P., Baumann, N., Brubakk, A. M., Evensen, K. A. I., Hovi, P., Kajantie, E., Lahti, M., Van Lieshout, R. J., Saigal, S., Schmidt, L. A., Indredavik, M. S., Wolke, D., & Räikkönen, K. (2017). Self-Reported Mental Health Problems Among Adults Born Preterm: A Meta-analysis. Pediatrics, 139(4), e20162690. https://doi.org/10.1542/peds.2016-2690
Mills, S. E. E., Nicolson, K. P., & Smith, B. H. (2019). Chronic pain: a review of its epidemiology and associated factors in population-based studies. British journal of anaesthesia, 123(2), e273–e283. https://doi.org/10.1016/j.bja.2019.03.023
Schubiner, H., Jackson, B., Molina, K. M., Sturgeon, J. A., Sealy-Jefferson, S., Lumley, M. A., Jolly, J., & Trost, Z. (2023). Racism as a Source of Pain. Journal of general internal medicine, 38(7), 1729–1734. https://doi.org/10.1007/s11606-022-08015-0
Zajacova, A., Grol-Prokopczyk, H., Liu, H., Reczek, R., & Nahin, R. L. (2023). Chronic pain among U.S. sexual minority adults who identify as gay, lesbian, bisexual, or "something else". Pain, 164(9), 1942–1953. https://doi.org/10.1097/j.pain.0000000000002891
